In 2009, when Hannah Perryman was diagnosed with multiple sclerosis (MS), she immediately thought of the hit TV series "The West Wing."
For the previous couple of months, the then-23-year-old had been suffering from optical neuritis, which causes dimmed vision and severe pain due to swelling in the nerves of the eyes. This condition is also an early sign of MS, a chronic disease that affects the central nervous system, including the brain, spinal cord, and optic nerves.
There is currently no cure for MS.
In that moment, at the doctor's office, Perryman's eyes weren't what she was most worried about. It was her legs.
"I knew nothing about MS except that I had recently watched an episode where the main character reveals that he has MS and can't stand up," she recalls. "I immediately said to my doctor, 'That's me. I'm going to end up in a wheelchair.'"
Nearly 1 million individuals are living with multiple sclerosis in the United States.
Convinced she had glimpsed her future, Perryman switched careers, opting for a desk job, and awaited the inevitable — a time when her mobility would be limited.
But as the years went by and Perryman's MS progressed, she realized the condition was eroding her health in different, unanticipated ways.
"There's a constant worrying of the unknown… the uncertainty with MS," she explains. "The depression and the swirling anxiety of getting one lesion in the wrong spot gets you mentally stuck."
Cognitive impairment affects up to 65% of people with multiple sclerosis — in every phase of the disease.
For Perryman, losing her train of thought while talking to friends or giving a presentation became routine. And when she'd try to speak, her thoughts would be a jumbled, unconnected mess.
This kind of forgetfulness, confusion, and trouble with concentrating, also known as brain fog, is common in people with MS, according to John DeLuca, a rehabilitation psychologist and the senior vice president for Research and Training at Kessler Foundation.
In fact, a decline in cognitive function is so prevalent that, on average, two out of every three people with MS experience it.
What is multiple sclerosis?
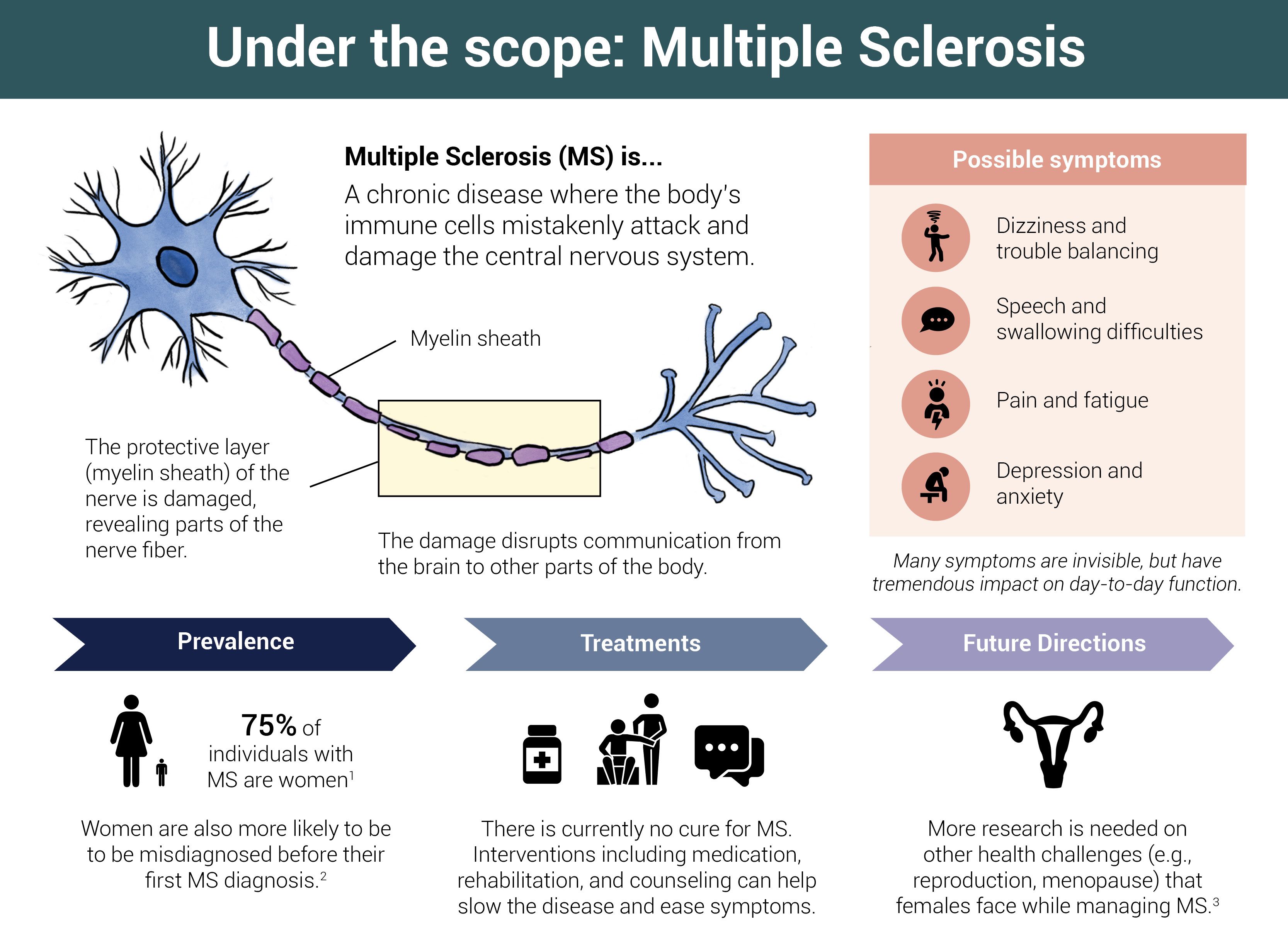
MS is a complex autoimmune disease affecting the central nervous system, leading to neurological symptoms. Like other autoimmune diseases, such as lupus, the body’s immune system mistakenly turns against itself and damages neural tissue.
MS affects about three times as many women as men. Some studies suggest the gender gap is growing, with more women being diagnosed than ever before, especially later in life.
Multiple sclerosis affects about three times as many women as men.
While MS can be diagnosed anytime, most people with MS receive a diagnosis between the ages of 15 and 50. For women, there are two notable peaks in the age of onset: late teens to early 20s and early 30s, when most women with MS experience their first symptoms or receive a formal diagnosis.
What are the different types of MS?
There are several types of MS, which describe how the disease manifests in a person over time. There is some evidence that MS evolves differently in men and women. For example, a recently published Danish study found more inflammatory activity in women with MS at a younger age. In contrast, men with the disease experienced more neurodegeneration and disability more quickly than women.
Clinically Isolated Syndrome (CIS): This term describes the first episode of neurological symptoms that may or may not develop into MS. To meet the definition of CIS, the episode must last at least 24 hours.
Relapsing-remitting MS (RRMS): RRMS is the most common type, affecting approximately 85% of people diagnosed with the disease. It is characterized by periods of relapses or flare-ups, during which new symptoms appear, or existing ones worsen. These relapses are followed by periods of remission, during which there is partial or complete recovery and a lack of disease progression.
Primary Progressive Multiple Sclerosis (PPMS): PPMS accounts for about 10-15% of MS cases and is characterized by a gradual and steady worsening of neurological function from onset. People with PPMS may experience occasional plateaus or temporary improvements, but the disease steadily progresses overall.
Secondary Progressive Multiple Sclerosis (SPMS): SPMS is a stage that some individuals with RRMS may transition into over time. Initially, people with RRMS experience relapses and remissions. But as the disease progresses, they may develop a more steady and continuous worsening of symptoms without relapses.
Understanding Cognitive Impairment in MS
Researchers attribute MS symptoms to damage to myelin, a protective covering that surrounds nerve fibers, leading to lesions in the brain, optic nerve, and spinal cord. The symptoms of MS vary depending on which part of the nervous system is damaged. The most common physical symptoms are fatigue; visual disturbances; tingling, numbness, or pins and needles in the face, limbs or trunk; muscle weakness or spasms; problems with coordination and balance; bladder problems; pain; and slurred speech.
But as Perryman’s experience makes clear, emotional, MS can also cause emotional and cognitive changes, including mood swings, anxiety and depression, and problems with memory, attention, and information processing.
“[Damage to the nervous system] can cause the brain to be less efficient and the processing speed to become slower,” says DeLuca. “And, over time, you may start to see problems in learning and memory.”

Why cognitive impairment in MS is overlooked
Even though cognitive decline is common among MS patients, the misconception persists that MS is primarily a condition affecting mobility and causing fatigue. And Perryman, among many others, had, at some point, believed that.
This misconception goes back to the turn of the 20th century when experts debated whether problems with cognition are a direct symptom of MS or a manifestation of other problems accompanying the condition, such as anxiety and depression.
"The father of MS identified problems in learning, memory, and information processing speed as a feature of the disease 150 years ago," DeLuca explains. "But medical students were taught in the '60s and '70s that there are no cognitive problems in MS, even though patients might say, "I'm really having a problem with my thinking." "
Paying attention to cognitive impairment in MS
Today, after years of research suggesting that cognitive decline is, in fact, a debilitating symptom of MS, healthcare providers are finally listening. Cognitive screening is becoming more common in MS clinics, and researchers are working to develop cognitive monitoring methods and effective interventions.
And the even better news: There are ways, outside of drug therapies, to develop coping skills and regain cognitive function.
The U.S. National Multiple Sclerosis Society has put together a guide to managing cognitive decline, which suggests people with MS:
Find a community of people with whom to share their fears and struggles. This can alleviate feelings of isolation, which are common after a diagnosis.
Seek psychological counseling. Emotional distress often runs hand in hand with cognitive issues and can worsen them.
Build up the brain's resilience, or cognitive reserve, by engaging with the world, reading, having stimulating conversations, and indulging in activities you love and enjoy.
How to improve your cognitive function
Various activities can help improve cognitive function. Some are therapeutic, while others are designed to help you compensate for cognitive abilities that have become impaired. The MS Society recommends the following:
Therapeutic activities
Combine learning modes: You will be more likely to remember something if you “see it, say it, hear it, write it, do it.” It’s okay to give yourself extra time.
Repeat and verify: Say what you hear and ensure it is correct to improve your attention and memory.
Spaced rehearsal: Repeat and practice information at intervals to improve your ability to store information.
Build associations: Use memory aids! For example, to remember the name of someone you just met, associate it with a friend or family member of the same name, or with a place, color, or event that sounds like it.
Compensatory activities
Consolidate and centralize: Designate one place in your home as information “Grand Central.” Include your master calendar, mail, bills, phone messages, keys, wallet and to-do and shopping lists.
Plan. Post a large calendar to display everyone’s appointments, activities, social engagements and reminders. Keep pens or markers hanging right beside it. Or use a computer program set up with reminders for routine tasks. (Synchronize it with your mobile devices so you have your appointments with you while on the go.)
Record. Dictate your to-do list, notes or other information to remember on a digital voice recorder (available on many phones).
Remind. Use checklists, the alarm on your watch or phone, your kitchen timer and more.
Eliminate or remove yourself from distractions. Turn off the TV, music and whatever else is “on” when speaking with someone in person or on the phone. Background visual and noise distractions can make learning or remembering more difficult. If you can’t eliminate the distraction (for example, people talking at a party), ask, “Can we talk in a quieter place?”
Take a break. If you are having difficulty concentrating, take a breath and refresh.
Do one thing at a time. Avoid switching back and forth from one topic or task to another. Finish what you’re working on or find an appropriate stopping place before switching to something else.
Where is more research needed on cognitive impairment in MS?
While considerable progress has been made in understanding these cognitive issues, several major research questions still need to be answered. Here are a few:
- What risk factors contribute to the development and progression of cognitive impairment in MS?
- What role does lifestyle play in cognitive decline in MS?
- How does cognitive impairment evolve over time in people with MS?
- Can reliable biomarkers or cognitive tests be developed to predict the risk of cognitive impairment in the early stages of MS?
- What role does cognitive reserve play in mitigating cognitive decline in MS, and how can individuals build or enhance cognitive reserve?
- What are the most effective treatment strategies for managing cognitive impairment in MS?
- What is the impact of disease-modifying therapies on cognitive function in MS?
- What are the most effective activities for improving cognitive function in MS?