
Women are almost twice as likely as men (31% vs 17%) to say they rarely or never wake up feeling well-rested, according to a recent survey by the American Academy of Sleep Medicine (AASM).
"The quality of our sleep is impacted by a number of internal and external factors, including stress, health, diet, timing, and the amount of time spent on sleep, as well as resources, which all play a role in determining how we feel when we wake up," said Dr. Kin Yuen, a sleep medicine specialist and AASM spokesperson in a statement.
"Many women embrace a 'do it all' mentality, whether they feel rested and rejuvenated or not. It is important for women to prioritize getting seven or more hours of sleep per night for their overall health," she said.
The survey underscores that women typically report poorer quality and more disrupted sleep across various life stages than men. They are also more likely than men to experience insomnia, a sleep disorder that can seriously impact women's physical and mental health, not to mention their social and professional lives.
This article will delve into insomnia, explore its causes and consequences, and provide practical tips to help women get the sleep they need.
This is a living article. The wmnHealth team will update it as new information becomes available.
 The prevalence rate of insomnia varies greatly depending on age, gender, marital status, income, and educational level. Source: National Sleep Foundation
The prevalence rate of insomnia varies greatly depending on age, gender, marital status, income, and educational level. Source: National Sleep Foundation
What is Insomnia?
Insomnia is a sleep disorder characterized by difficulties falling asleep, staying asleep, or waking up earlier than desired. It can make a person tired, irritable, and unproductive during the day.
Insomnia
"Difficulty in initiating or maintaining a restorative sleep, which results in fatigue, the severity or persistence of which causes clinically significant distress or impairment in functioning. Such sleeplessness may be caused by a transient or chronic physical condition or psychological disturbance."
Source: American Psychological Association's Diagnostic Manual
There are two types of insomnia: primary and secondary.
- Primary insomnia: This type of insomnia is often the result of lifestyle factors, stress, or poor sleep habits. It is not caused by any underlying medical condition or substance use.
- Secondary insomnia: This type results from underlying medical conditions like chronic pain, respiratory disorders, psychological problems, or neurodegenerative disorders, or from the side effects of medication.
Primary insomnia can be particularly frustrating because it seems to have no apparent cause. It can be a vicious cycle, where the more a person worries about not being able to sleep, the harder it becomes to fall asleep. This may lead to frustration and anxiety, exacerbating the problem and leading to sleepless nights.
While occasional sleepless nights are normal, chronic insomnia is a persistent condition that can significantly impact your quality of life. Insomnia becomes chronic when it persists for at least three nights a week over three months.
Signs and Symptoms of Insomnia

How Common is Insomnia in Women?
Approximately 1 in 4 women experience insomnia in their lifetime, though prevalence estimates vary from one research study to the next.
What's clear is that insomnia is more prevalent in women than men. A recent meta-analysis — an analysis combining the results of multiple research studies — found that insomnia is one-and-a-half times more likely to occur in women than men.
The Impact of Insomnia on Women's Health
Insomnia is more than an inconvenience. Over time, it can profoundly affect a person's health and well-being. For example, research has shown that chronic insomnia is associated with an increased risk of developing conditions such as obesity, diabetes, heart disease, and even certain types of cancer.
Insomnia has also been linked to mental health conditions, including anxiety and depression, and neurological conditions like cognitive impairment, multiple sclerosis, and Alzheimer's disease. For example, a study published earlier this year found that sleep disturbances like insomnia, sleep apnea, and sleepiness also contribute to cognitive decline in women with multiple sclerosis. Several other studies have found an association between impaired sleep and an increased risk of Alzheimer's. The relationship is strong enough that some researchers are exploring whether treating insomnia in patients with Alzheimer's could prevent or limit cognitive decline.

Research has also shown that sleep deprivation affects women differently than men, elevating their risk for serious physical health conditions like type 2 diabetes and heart disease. For example, women are more likely to develop hypertension, also known as high blood pressure, due to sleep deprivation.
Sleep deprivation also puts women's cognitive and mental health at risk. For example, researchers have found gender differences in cognitive tasks such as decision-making and risk-taking when adults are sleep deprived. In one study, sleep-deprived women were more risk-averse than women who got adequate sleep, while the opposite was true for sleep-deprived men. Chronic sleep deprivation has also been linked to an increased risk of developing depression and anxiety disorders. The lack of quality sleep can disrupt the brain's ability to regulate emotions and process stressful experiences.
Understanding the Factors Contributing to Insomnia in Women
Various factors contribute to this gender difference, including hormonal fluctuations, stress, chronic pain or medical conditions, the higher prevalence of mental health disorders in women, and lifestyle factors. Gender roles and responsibilities, such as caring for children and aging parents, can lead to stress and insomnia in women.
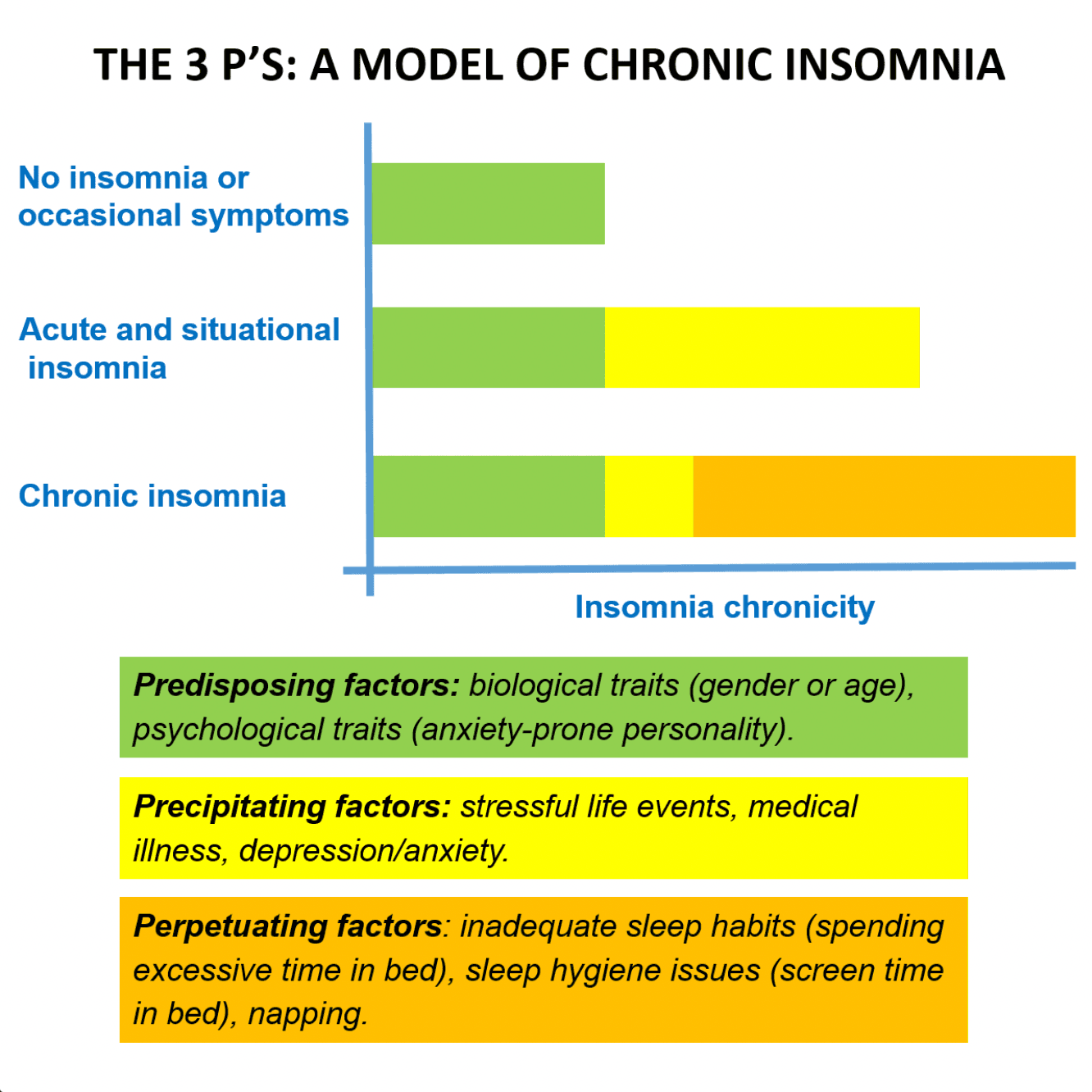 Source: Sleep On It Canada
Source: Sleep On It Canada
Recognizing the unique risks women face due to insomnia is crucial to develop effective strategies for prevention and treatment.
Let's explore some of the critical factors in more detail.
Stress, Anxiety, and Mood Disorders
Stress is one of the primary culprits behind insomnia in women. The demands of work, family, and personal life can put significant pressure on women, making it difficult to relax at night.
Anxiety and mood disorders such as depression, which are more common in women than men, can also disrupt sleep. These psychological factors can cause racing thoughts, restlessness, and an overall sense of unease, making it challenging to achieve restful sleep.
Elevated stress levels can also trigger hormonal imbalances and physiological responses that interfere with sleep.
Hormonal Changes
Women experience various hormonal changes throughout their lives, and these fluctuations can significantly impact sleep patterns because hormones play a crucial role in regulating sleep-wake cycles.
Reproductive years: For example, many women report difficulty falling or staying asleep due to hormonal shifts during the menstrual cycle. Women often experience more sleep disturbances during the premenstrual and menstrual phases.
Pregnancy: Pregnancy brings sleep challenges, including discomfort, frequent bathroom trips, and hormonal changes affecting sleep quality. These factors can make it difficult for pregnant women to get the restful sleep they need.
Menopause: During menopause, women undergo significant hormonal, as well as other physical and psychological changes, which can lead to insomnia. In fact, one study pegged the occurrence of insomnia during menopause among women at 39% to 47%. Hot flashes and night sweats are common menopausal symptoms that can disrupt sleep patterns.
Chronic pain or medical conditions
Chronic pain, including back pain, and medical conditions such as arthritis can cause insomnia in women.
These conditions can cause discomfort and pain, making it difficult to fall asleep and stay asleep.
Certain medications
Medications that can cause insomnia in women include:
- Antidepressants
- Steroids
- Asthma medication
- Blood pressure medication
- Thyroid hormone medication
Despite the widespread use of oral contraceptives in women, research is limited on their sleep.
Lifestyle factors
Lifestyle factors that contribute to insomnia in women include:
- Irregular sleep schedules,
- Lack of physical activity,
- Drinking caffeinated beverages or alcohol, or eating big meals close to bedtime,
- Using electronic devices before bedtime can contribute to insomnia in women.
Why Sleep Isn't Equal for Everyone
In addition to women, in the U.S., people of color are disproportionately affected by poor sleep health and sleep disorders. In a position statement on sleep health equity, National Sleep Foundation lists the following potential contributors:
- Racial discrimination: Research has uncovered an association between experienced discrimination and poor sleep health.
- Access to care: Black individuals are less likely to be diagnosed and treated for sleep conditions despite being at higher risk.
- Financial distress: People of color experience higher levels of unemployment and poverty, which contribute to day-to-day stress.
- Neighbourhood environment: Pollution, noise, allergens, and other stressors in neighborhoods with a higher percentage of underrepresented individuals can contribute to insomnia.
- Shift work: Underrepresented populations are more likely to work night shifts or irregular or extra hours that are more likely to disrupt sleep schedules.
- Occupational hazards: Many people of color report safety risks and job stress from discrimination in the workplace.
Source: National Sleep Foundation
How does sleep change as women age?
As women age, changes in sleep patterns are common. Total sleep time, efficiency, and deep sleep, the most restorative sleep phase, decrease with aging. Older women may experience difficulty falling asleep, maintaining sleep, and waking up earlier than desired. These changes are part of normal aging and tend to peak around age 60, then stabilize.
But sleep changes associated with aging are often multifactorial. Medical conditions, psychological disorders, sleep disorders such as sleep apnea and restless leg syndrome, and changes in social engagement, lifestyle, and environment commonly accompany aging and affect how we sleep.
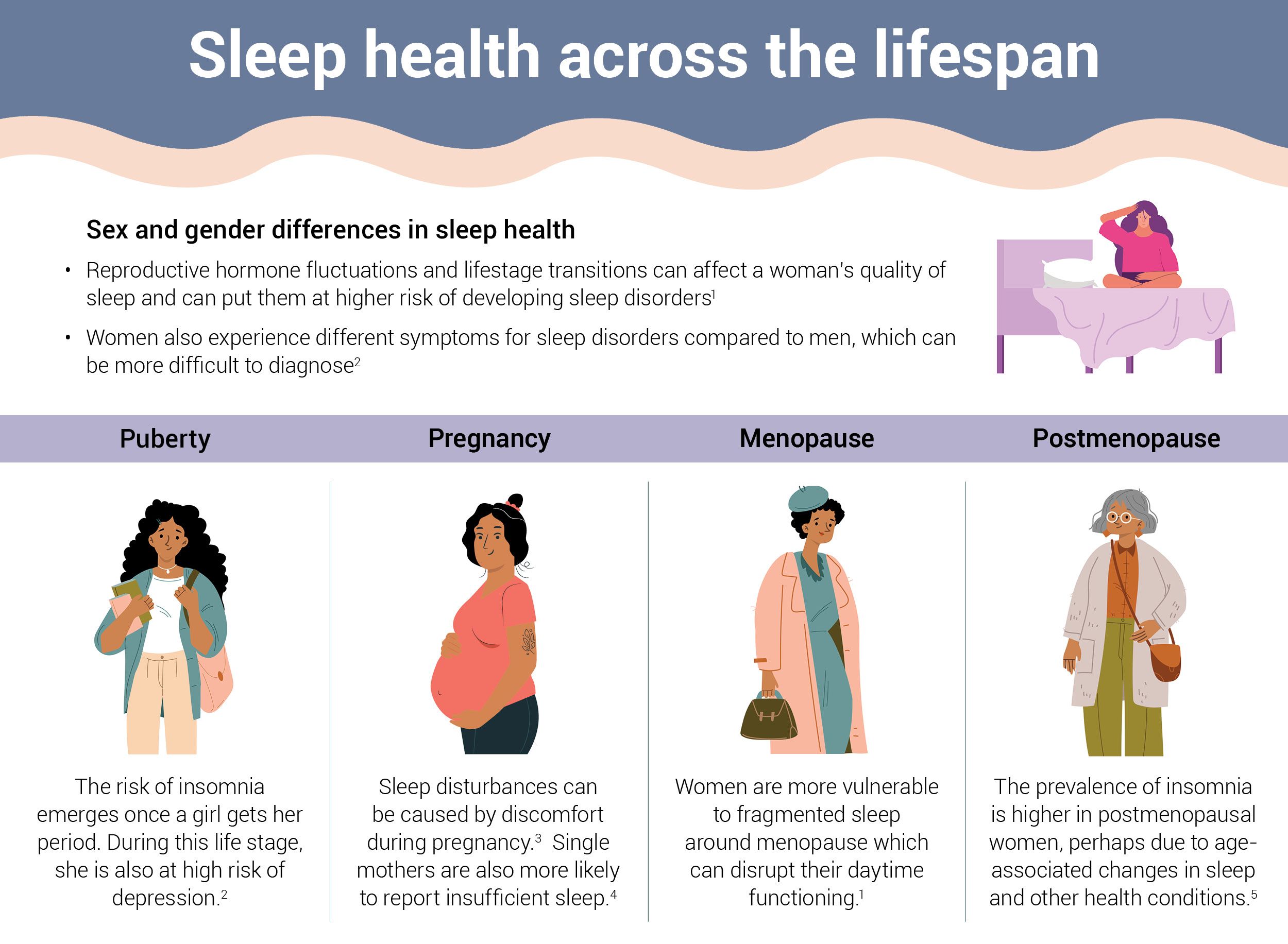 Infographic by Cat Lau. (References below. Illustrations from Vecteezy.com)
Infographic by Cat Lau. (References below. Illustrations from Vecteezy.com) Treating Insomnia
The key to overcoming insomnia is to address the underlying causes and develop healthy sleep habits. This may involve changing your sleep environment, establishing a regular sleep schedule, changing your thoughts and beliefs related to sleep, practicing relaxation techniques, and managing stress.
Here are the most common and effective therapies for insomnia.
Cognitive-behavioral therapy for insomnia (CBT-I)
CBT-I is a form of talk therapy that helps people with insomnia change their negative thoughts, beliefs, and behaviors related to sleep. CBT-I helps individuals develop healthy sleep habits and learn practical techniques to improve sleep quality.
It is a highly effective treatment for chronic insomnia. In fact, studies show that CBT-I is more effective than sleep medication alone in treating chronic insomnia. As a result, it is the recommended first-line treatment for adults with the sleep disorder.
CBT-I consists of a combination of treatments that include cognitive therapy around sleep, behavioral interventions such as sleep restriction, stimulus control and relaxation techniques, and education such as habits for a good night's sleep.
CBT-I can be conducted through individual or group therapy sessions, telephone or web-based modules, and/or self-help books.
Medications
In addition to therapy, some medications can help with insomnia. However, these should be used as a last resort and in consultation with a healthcare professional. Sleep medications can be effective in the short term but are not a long-term solution and can have serious side effects.
According to the National Sleep Foundation, medications that can be used to treat insomnia include:
- Benzodiazepine sedatives and non-benzodiazepine sedatives. These work to help people fall asleep. Examples of benzodiazepine sedatives are triazolam, estazolam, temazepam, flurazepam, and quazepam. Examples of non-benzodiazepine sedatives are zolpidem, eszopiclone, and zaleplon.
- Orexin receptor antagonists affect the action of the hormone orexin (chemicals involved in regulating the sleep-wake cycle) in the brain to help you sleep. Examples of orexin receptor antagonists include suvorexant and lemborexant.
- Low-dose doxepin works to block histamine receptors. It is intended for people who have trouble staying asleep to continue sleeping.
- Ramelteon is another insomnia medication that works differently than other sedative medications by affecting melatonin receptors. It is designed specifically to help people fall asleep.
Natural remedies
There is widespread interest in the use of melatonin supplements for the treatment of insomnia. Melatonin is a hormone that your brain produces in response to darkness.
Melatonin supplements are made from animals or microorganisms or synthetically.
According to the U.S. National Institutes of Health, melatonin supplements may be helpful for sleep problems caused by shift work or jet lag. It may also be helpful for people with insomnia, but its effect is small. Melatonin appears to be safe in the short term, but its long-term safety has yet to be proven.
Very little evidence demonstrates that other natural remedies like herbal teas, aromatherapy, supplements such as kava or valerian, or acupuncture are effective treatments for insomnia.
According to the U.S. National Institutes of Health, there is some preliminary evidence that yoga and massage therapy may be helpful for insomnia, particularly in postmenopausal women.
When to Seek Professional Help for Sleep Problems
Suppose you've tried various self-help strategies but continue to struggle with sleep. In that case, it may be time to seek professional help. A sleep specialist can help diagnose and treat underlying sleep disorders contributing to your insomnia.
Keep track of your sleep patterns and any related symptoms to share with your healthcare provider. They may recommend a sleep study to evaluate your sleep quality further and identify potential sleep disorders.
Practical Tips for Better Sleep
The American Academy of Sleep Medicine recommends the following tips to establish healthy sleep hygiene and improve the overall quality of sleep:
- Keep a consistent sleep schedule. Get up at the same time every day, even on weekends or during vacations.
- Make your bedroom quiet and relaxing. Keep the room at a comfortable, cool temperature.
- Limit exposure to bright light in the evenings and turn off electronic devices at least 30 minutes before bedtime.
- Exercise regularly and maintain a healthy diet.
- Avoid consuming caffeine, nicotine and alcohol before bedtime.
- If you don't fall asleep after 20 minutes, get out of bed. Do a quiet activity without much light exposure until you feel sleepy.
Resources:
- The American Academy of Sleep Medicine’s website on Sleep Education, includes information and tips on healthy sleep in women: https://sleepeducation.org
- The National Sleep Foundation’s infographic, “6 Steps to Healthy Sleep”: https://www.thensf.org
- Sleep On It Canada offers sleep diaries, peer support groups, online programs, podcasts and videos about sleep: https://sleeponitcanada.ca



