Dec 05, 2023, 5:00 am UTC
5 min
Created by
Gut-Brain Connection: How bacteria in the gut play a role in neurodegeneration
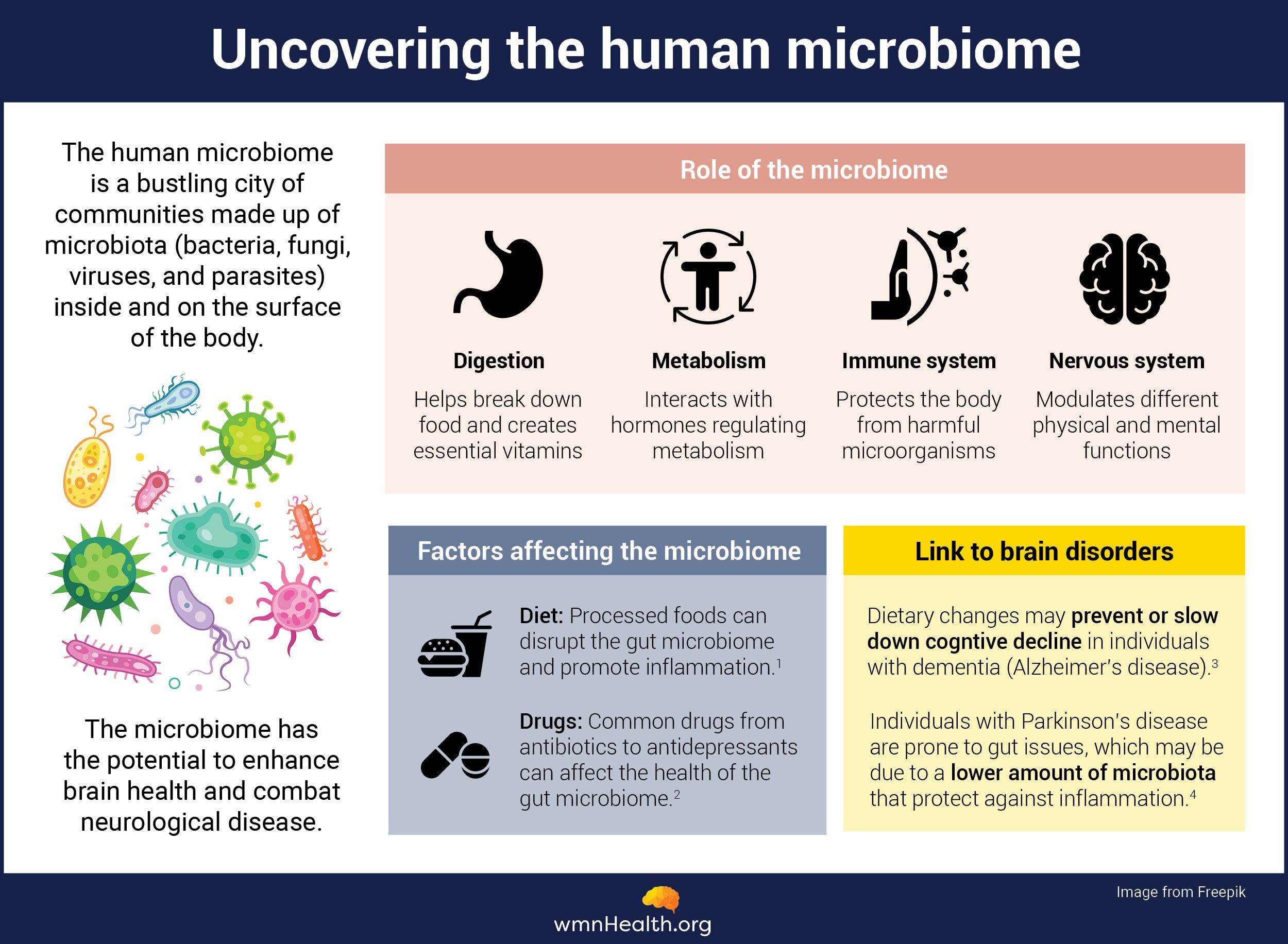
The gut is packed with billions bacteria, fungi, and other microorganisms that influence human health and disease.
This collection of microorganisms, known as the gut microbiome, is a complex community that changes over time and across life stages. Factors like genetics, sleep, diet, and exposure to stress or medications can drastically shift its composition, affecting not only digestion, metabolism, and immune response but also behavior and brain function.
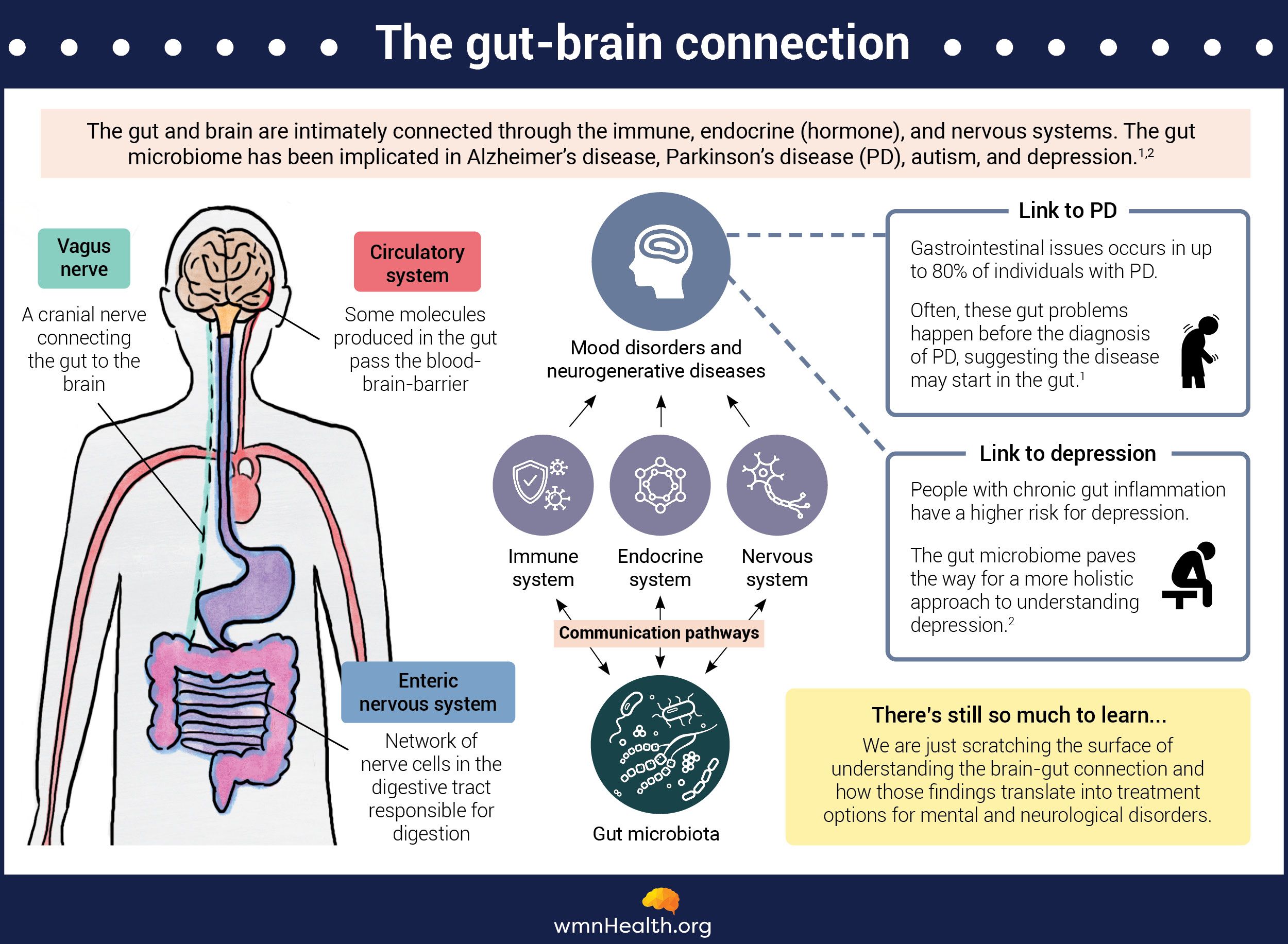
This is all thanks to an intricate network of proteins, neurons, and chemicals that connects the gut to the emotional and cognitive centers of the brain, forming a two-way communication highway known as the "gut-brain axis."
Emerging research suggests this communication highway also plays a critical role in how neurodegenerative conditions like Alzheimer's and Parkinson's arise and progress.
 Infographic by Cat Lau. (References below.)
Infographic by Cat Lau. (References below.)Could gut bacteria be an early indicator of Alzheimer's disease?
One afternoon, at a children's soccer game, microbiologist Gautam Dantas started chatting with his colleague Beau Ances, a neurologist at the Washington University School of Medicine who specializes in studying and treating people with Alzheimer's disease. Their conversation gave birth to a research project investigating a possible link between the gut and the brain: the gut microbiome of people with preclinical Alzheimer's disease (AD).
"Brain changes in AD start well before cognitive symptoms show up, so think of preclinical Alzheimer's as an inflection point — you have the disease but not the symptoms," Dantas explains. "We thought, could it be possible there are markers of Alzheimer's in the gut that would allow experts to intervene early in the disease process?"
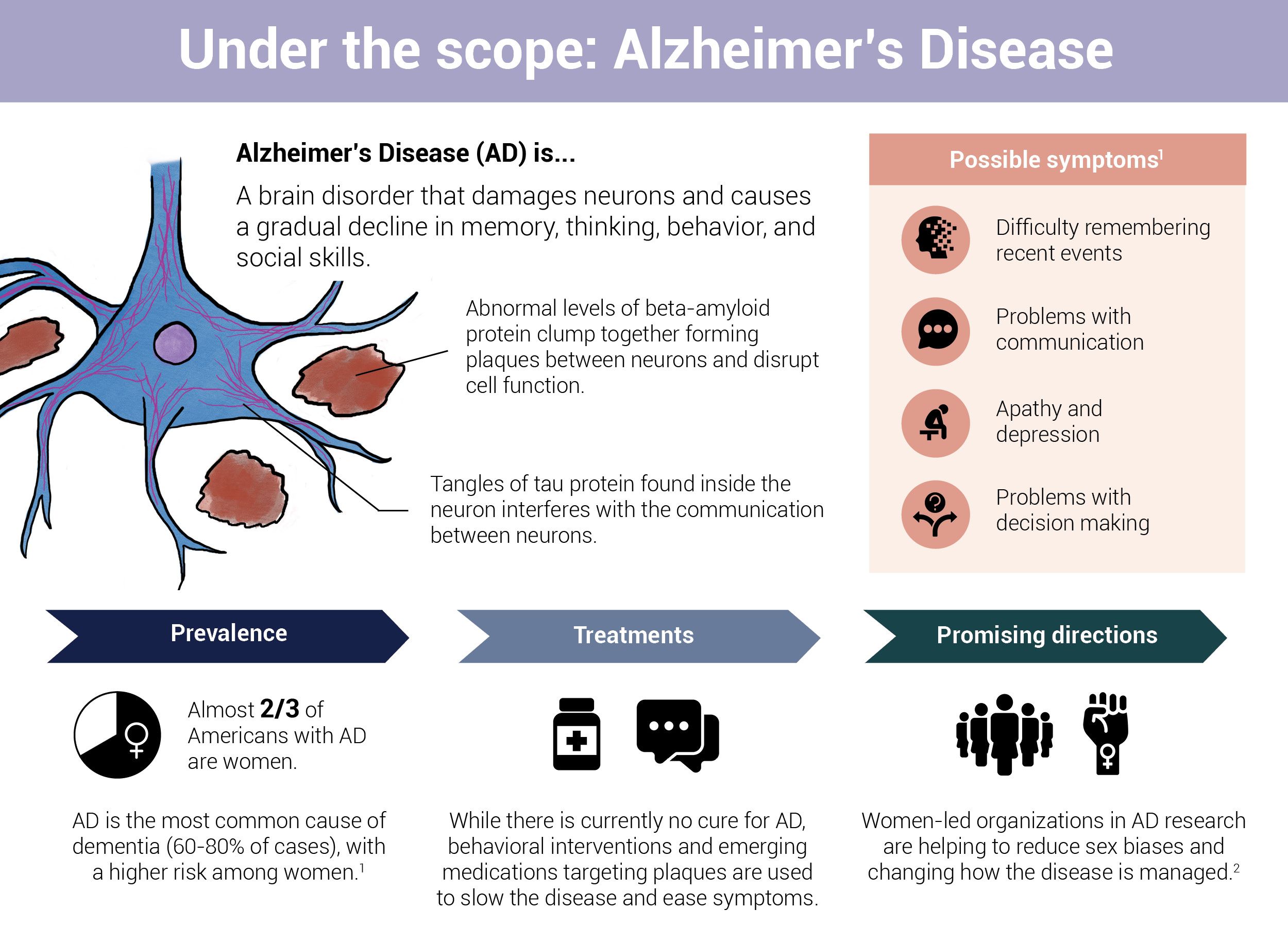
In the early stages of Alzheimer's disease, tau proteins begin to clump together into tangled strands inside axons, nerve cells' hair-like extensions. At the same time, an overproduction of the amyloid beta protein eventually leads to the formation of clusters that erode the connections between nerve cells. Indeed, this gradual buildup of proteins in the brain can go unnoticed for decades before hallmark symptoms of the condition appear — impaired cognition, including challenges with memory and thought processing. While prior studies have found changes in the gut microbiome of people with advanced-stage Alzheimer's, the role of gut bacteria, especially in the early stages of the disease, remains a mystery.
 Infographic by Cat Lau. (References below.)
Infographic by Cat Lau. (References below.)To investigate if the gut could be harboring early clues of Alzheimer's disease, Dantas and his colleagues conducted brain scans and sampled cerebrospinal fluid to look for signs of Alzheimer's in 164 participants with no symptoms of cognitive impairment. The results revealed that about a third of them had preclinical Alzheimer's.
Then, the researchers compared the gut bacteria in stool samples taken from people with preclinical AD to those of healthy controls. The analysis showed that species of the bacteria present in the gut of people with preclinical Alzheimer's were markedly different: They had larger populations of bacteria responsible for breaking down the amino acids arginine and ornithine, which facilitate the buildup of amyloid beta. On the other hand, healthy individuals had higher numbers of bacteria that regulate glutamate levels, protecting nerve cells from over-activation.
Nearly two-thirds of Americans living with Alzheimer’s are women
Just as Dantas and Ances suspected, the results confirmed a link between the composition of gut bacteria and Alzheimer's disease. These changes could potentially serve as a more accessible and less invasive screening tool for the condition than brain scans and spinal taps.
However, these findings raise many more questions: Is the gut influencing the brain or the brain influencing the gut? How does the microbiome composition change across different stages of the disease? Could altering the composition of the bacteria in the gut change the course of Alzheimer's? The researchers are hoping to answer some of these questions with a five-year-long follow-up study that is currently underway.
Dantas says one thing is clear for now: "The microbiome is an organ, not an accessory element. And you can make some very hardcore changes [to it] with pretty minimal effort. But the silver lining is that it's also an opportunity."
 Infographic by by Cat Lau. References below.
Infographic by by Cat Lau. References below.Does Parkinson's disease start in the gut?
Constipation, cramping, and bloating are some of the most common symptoms of Parkinson's disease manifesting early in the condition — before motor symptoms emerge. Yet for decades, experts focused on identifying Parkinson's origins have focused on other, mainly neurological mechanisms. Now, with a slew of studies teasing out the gut-brain connection in Parkinson's, a hypothesis that first emerged two decades ago is slowly gaining credence: The disease may start in the gut.
"When this paper [hypothesizing the Parkinson's-gut connection] came out, the concept of gut microbiome influencing the brain wasn't developed. But the idea that a brain condition could start outside the brain intrigued me," says Livia Hecke Morais, a neurobiologist and postdoctoral scholar at California Institute of Technology, whose work focuses on understanding the gut microbiome's and Parkinson's disease.
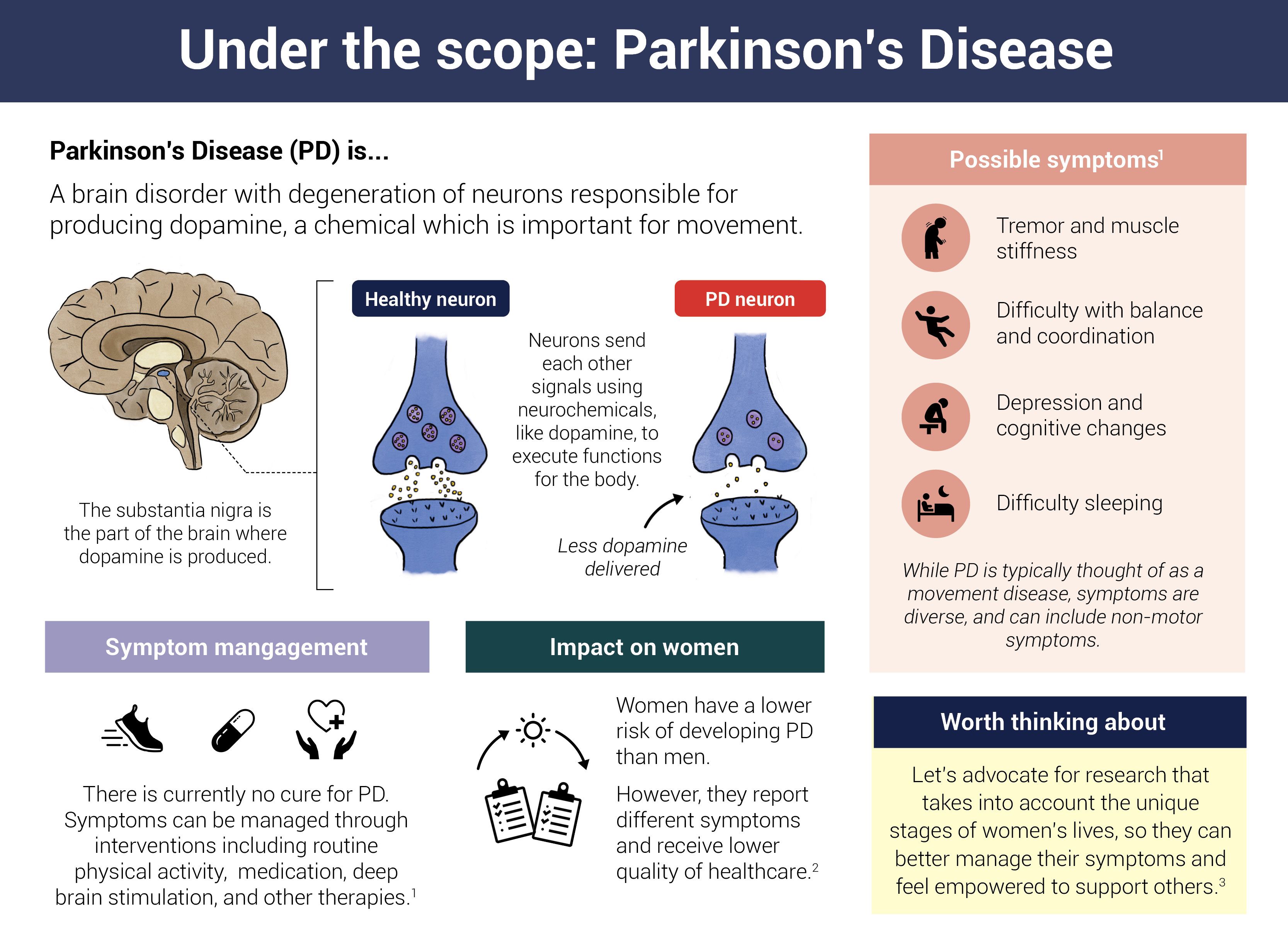
Like many other neurodegenerative conditions, clumps of misfolded proteins are at the heart of Parkinson's. Over time, these proteins form toxic clusters called Lewy bodies that kill off dopamine-producing neurons in the brain, leading to movement problems and cognitive changes.
 Infographic by Cat Lau. (References below.)
Infographic by Cat Lau. (References below.)In 2019, neurologists at Johns Hopkins University tested the hypothesis that these protein clumps first form in the gut and cause neighboring proteins to misfold, sparking a chain reaction that spreads all the way to the brain through the vagus nerve.
When the researchers injected misfolded alpha-synuclein protein in the guts of mice, they found that the proteins slowly spread to regions of the brain implicated in Parkinson's disease. The injected mice also began to show symptoms of the condition — they performed worse on movement, strength, and memory tests than mice that hadn't received the misfolded proteins.
This work implicated the gut in Parkinson's disease and sparked several important questions, including what triggers the initial gastrointestinal changes that ignite the spread of the disease?
Researchers at Columbia University say they have a clue.
In a recent paper, the researchers injected misfolded alpha-synuclein protein in the guts of genetically modified mice. They found that small portions of these misfolded proteins made neurons vulnerable to a harsh immune attack that left them severely damaged. This immune response, the experts believe, is what kick-starts the condition: In the study, the brains of injected mice didn't develop signs of the condition, but the mice began to experience gastrointestinal symptoms, such as constipation, that appear in the early stages of Parkinson's disease.
According to Morais, who was not involved in the research, the gut-brain connection is just one piece of the puzzle in the biology of Parkinson's disease. But the bottom line, she says, is "it's just easier to manipulate the gut than the brain. Hopefully, with more biological evidence, we can develop drugs that target the gut microbiome to diagnose and treat neurodegenerative diseases."
Infographic References
Human Microbiome
- Song Z, Song R, Liu Y, Wu Z, Zhang X. Effects of ultra-processed foods on the microbiota-gut-brain axis. Food Res Int. 2023 May;167:112730.
- Vich Vila A, Collij V, Sanna S, Sinha T, Imhann F, Bourgonje AR, Mujagic Z, Jonkers DMAE, Masclee AAM, Fu J, Kurilshikov A, Wijmenga C, Zhernakova A, Weersma RK. Impact of commonly used drugs on the composition and metabolic function of the gut microbiota. Nat Commun. 2020 Jan 17;11(1):362.
- Romanenko M, Kholin V, Koliada A, Vaiserman A. Nutrition, Gut Microbiota, and Alzheimer's Disease. Front Psychiatry. 2021 Aug 5;12:712673.
- Romano S, Savva GM, Bedarf JR et al. Meta-analysis of the Parkinson’s disease gut microbiome suggests alterations linked to intestinal inflammation. npj Parkinsons Dis. 7, 27 (2021).
Alzheimer's disease
- 2023 Alzheimer's Facts and Figures: Special Report, Alzheimer's Association (Accessed June 20, 2023)
- Castro-Aldrete L, Moser MV, Putignano G, Ferretti MT, Schumacher Dimech A and Santuccione Chadha A (2023) Sex and gender considerations in Alzheimer’s disease: The Women’s Brain Project contribution. Front. Aging Neurosci. 15:1105620.
Gut-brain connection
- Morais, L.H., Schreiber, H.L. & Mazmanian, S.K. The gut microbiota–brain axis in behaviour and brain disorders. Nat Rev Microbiol 19, 241–255 (2021).
- Flux, M.C., and C.A. Lowry. Finding intestinal fortitude: Integrating the microbiome into a holistic view of depression mechanisms, treatment, and resilience, Neurobiology of Disease, Volume 135, 2020, 104578.
Parkinson's disease
- Parkinson's Disease, National Institutes of Health (Accessed June 9, 2023)
- Women and PD, Parkinsons.org (Accessed June 9, 2023)
- Subramanian, I., et al. Unmet Needs of Women Living with Parkinson's Disease: Gaps and Controversies. Movement Disorders, Vol. 37, No. 3, 2022